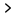Brain injury and brain damage are results of the destruction of specific brain cells–or neurons. Injuries can occur externally, like through a fall or physical trauma, or from an internal cause. The term traumatic brain injury is when you sustain damage to the brain due to external forces. The leading causes of TBI are sports, physical violence, firearms, automobile accidents, and falls. Severe TBI can result in both mortality and long-term disability.
It isn’t just the initial brain injury that leads to adverse outcomes. TBI is linked to a host of secondary conditions such as paralysis, poor coordination, seizures, post-traumatic epilepsy, hydrocephalus or an accumulation of brain fluid, and behavioral changes.

What Qualifies Someone as Having Post-Traumatic Epilepsy?
Typically, when you sustain a TBI, if you are likely to have a seizure, you will do so during the early phases within a week of the injury date. However, seizures can also appear later on. When seizures occur early on, they must be treated immediately to prevent further brain damage. Later seizures are those which occur more than a week after the injury and tend to become recurrent. If they happen more than once, technically, they qualify as “post-traumatic epilepsy.”
Seizures occur when the electrical discharge of the brain is abnormal. The symptoms can be as benign as staring and being unresponsive to severe, such as shaking of the arms, legs, head, and body. They can also affect all of the senses, leading to strange tastes, visual images and hearing odd sounds. Patients can also experience changes in their olfactory senses. There are also cases where the person is incapable of understanding others or responding to them.
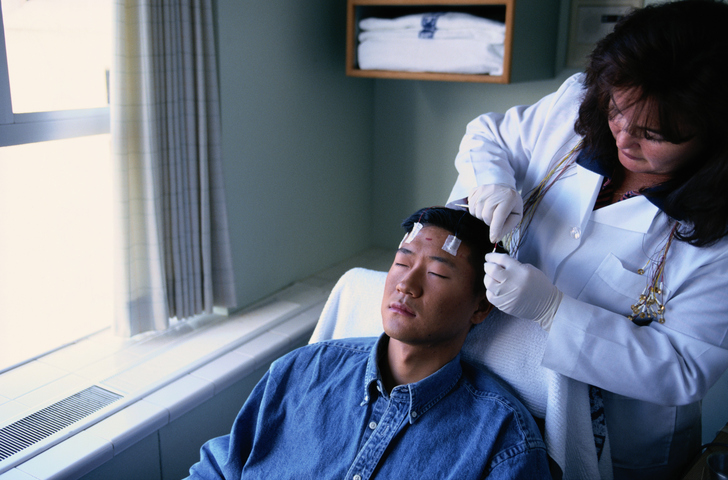
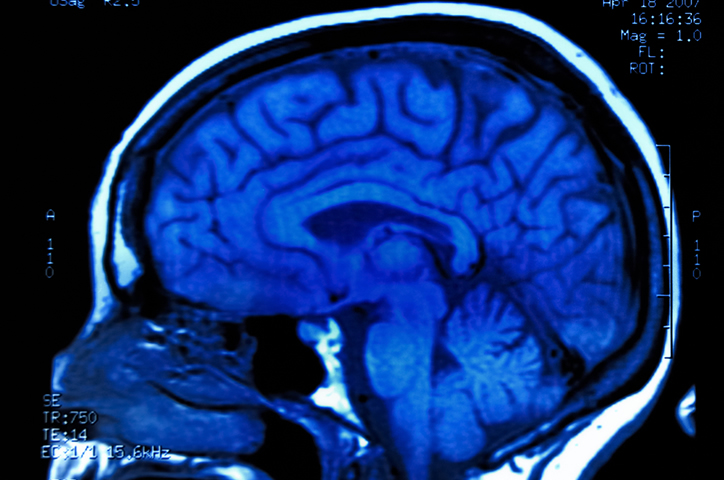
TBI is the highest risk factor of epilepsy in people of ages 15 to 24. Specifically, post-traumatic epilepsy stems from a localized, or focal, injury. Typically, the temporal and frontal lobes are the ones that sustain damage. The likelihood of developing TBI is relative to the severity of the injury. Risks increase according to occurrences of intracranial hematoma or bleeding in the brain, skull fractures, and if a patient is in a coma for more than a 24 hour period. The best way to diagnose a TBI is through MRI imaging.
How to Prevent Long-Term Post-Traumatic Epilepsy
The best prevention of post-traumatic epilepsy is through the use of anti-seizure medications. Anti-seizure meds can help decrease the frequency of seizures early on, but they may be ineffective in preventing those which occur long after the initial injury.
80% of people who have post-traumatic epilepsy will have seizures within two years after the injury. After five years, the risks decrease substantially, with as many as half of those who have brain injuries going into spontaneous remission and no longer requiring treatment. The only time that a patient with PTE would need to visit a hospital is if the seizures last longer than five minutes or if the treatment is not working. Patients who have PTS, for whom treatment has not been successful, should be EEG monitored and evaluated to find a treatment that works for them.
Featured Image Source: Thinkstock/Keith Brofsky
Sourced from: epilepsy.com